Table of Contents
Clinical scenario
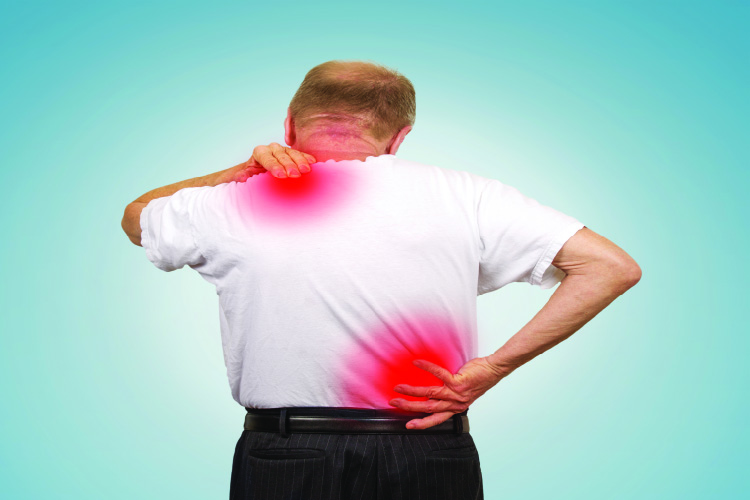
Madam Kim is a 75 years old lady who presented to a public hospital with a painful right hip after a trivial fall at home. She was diagnosed to have a fracture of the neck of right femur. She was then advised for a surgical procedure to fix the fracture bone which she agreed upon. However due to the long waiting list of at least two weeks in the public hospital before the surgery can be performed, Madam Kim opted for treatment in a private hospital instead.
A partial hip replacement surgery was carried out and Madam Kim recovered well from the surgery soon after. She was prescribed with a medication to reduce the risk of recurrent fracture during her follow up appointment in which she was compliant for a brief period of time. She did not return for subsequent follow up and it is not known if she continues taking the medication prescribed.
Scope of the problem
Ageing population
This is a common clinical scenario in our community as far as osteoporosis care and prevention is concerned. The word osteoporosis literally means “porous bones”. In simple term it means that the bone becomes brittle and weak, making it susceptible to fracture when trivial trauma or minimal force applied. Common osteoporotic fractures include neck of femur fracture, vertebral compression fracture and distal radius fracture. These fractures are commonly seen in our healthcare system as the society ages and the life expectancy of the population increases.
A data provided by Asia Pacific Osteoporosis audit of Malaysia in 2013 shows that over the next four decades, the number of Malaysian population aged over 70 years is expected to increase by 417%. This shows an increment in number from 939,010 in 2013 to 4.8 million in 2050. The life expectancy will also increase seven-years longer than today, rising from 74 years to 81 years. The graph shown below (Figure 3) explains the rapid decline of bone density with age which is the hallmark feature of osteoporosis.
This phenomenon is seen more markedly in women compared to men especially after the age of 50. The increased number of Malaysia’s greying population would mean osteoporosis and its complications would be a significant burden in our healthcare system. It is estimated that osteoporosis will result in 1 in 3 women and 1 in 5 men to have fracture. In Malaysia the cost of fracture treatment is increasing. Some Malaysian data have shown that a cost of operative surgery for a hip fracture is around USD 6000 in private healthcare. It is much cheaper in public hospitals but the waiting list may take around two weeks or more.
Who else are at risk?
Apart from increasing age there are also several other factors that contributes to the development of osteoporosis. These factors are further divided into two broad categories namely non-modifiable and modifiable factors.
Non-modifiable factors
1. Advancing age
2. Ethnic group (Oriental & Caucasian)
3. Female gender
4. Premature menopause (< 45 years)
5. Slender build
6. Family history of osteoporosis in first degree relative
Modifiable factors
1. Low calcium intake
2. Sedentary lifestyle
3. Cigarette smoking
4. Excessive alcohol intake
5. Excessive caffeine intake
What can be done?
Health education
As in any other significant health problems the key for successful intervention is to increase the awareness level of our community through health educations. Healthcare professionals too need to be aware of this as they are one of the key players in educating patients regarding osteoporosis. Health campaigns at every level need to be done regularly by health authorities as well as non-governmental organisations. Public needs to be educated about osteoporosis in general, its risk factors, screening test available and prevention as well as treatment.
Screening tests
Bone mineral density (BMD) is a screening tool for osteoporosis. The hallmark of osteoporosis is when there is a significant reduction in BMD in certain areas of our body. This test can be easily done with various instruments and it is affordable as some centres provide this test for free. In general there are two main screening modalities used in Malaysia for BMD namely DEXA or dual energy X-ray absorptiometry and quantitative ultrasound. The former test is the gold standard and widely available in many hospitals and in some health screening centres in Malaysia. The ultrasound test is becoming popular as it is portable and can be used for screening in health promotion activities at shopping malls and work places.
DEXA scan is used to screen those who are at risks. If the test results show that an individual has a significant low bone density, then he or she need to be started on treatment. DEXA scan is also used to monitor those individuals that are already on treatment; every 1-2 years after treatment starts. QUS on the other hand does have a role in mass public screening but any abnormal test needs to be verified by a health professional most of the time together with a DEXA scan result.
There are other tests such as biochemical blood test which measure the formation and resorption of bone but they are mainly for treatment monitoring and not for making a diagnosis of osteoporosis.
Prevention of osteoporosis
Many studies have shown that osteoporosis may be prevented and in those who have established osteoporosis, its complications such as fracture can be prevented by taking several steps.
Calcium intake
In osteoporosis there is a net loss of calcium from our body and evidence has shown that an adequate intake of calcium is positively correlated with good bone mass. What is the adequate level of calcium intake? It varies according to age, gender and physiological status as shown in the table nex page.
It is recommended that daily calcium intake is taken in the food form, however calcium supplement is strongly advised if daily calcium intake is inadequate. Calcium supplements come in various concentration therefore consultation with qualified professional is recommended.
Vitamin D intake
Vitamin D is an important element in the absorption of calcium from our gut. Those who are exposed to adequate sunlight (more than 15 minutes a day) should have adequate level of Vitamin D in their body but in individuals who are house bound, sedentary and so forth Vitamin D supplement is needed.
Exercise
Regular physical exercise is beneficial not only for cardiovascular health but in the prevention of osteoporosis too. Weight bearing exercise such as walking, hiking, jogging, climbing stairs and dancing is the best exercise for healthy bone. Needless to say any physical activity to be carried out need to discussed with relevant health professionals to avoid problems.
Pharmacological treatment
Other than calcium and vitamin D supplements there are specific medications that are used by doctors to prevent osteoporosis and reduce the risks of fractures in those patients with established osteoporosis. There are various types of medications can be used such as hormone replacement, selective oestrogen receptor modulators, biphosponates, strontium and parathyroid hormone. Studies have shown that medical treatment is cost-effective and recommended to those who are at risks of osteoporosis and its complications.
Prevention of falling
The most frequent cause of fractures in osteoporotic patients is related to a fall as shown in the clinical case described above. There are various factors that can contribute to falling, such as poor vision, poor balance, weak or painful limbs and joints which may be difficult to control and need advice from health professionals for them to overcome. There are also factors which are can be easily managed and this is frequently missed by patients and their caregivers. Household hazardous environment such as slippery floor, inadequate lighting, steps, damaged carpets with curled edges or loose and unsecured floor rugs is associated with slipping and tripping. It is important that this preventable cause of fall is made aware to patients and their caregivers to reduce the risks of falling and possibly fractures.
Conclusion
The incidence of osteoporosis is on the rise and it will have a big impact on healthcare. Awareness of the members of the public is very much important in reducing the negative impact of osteoporosis. The role of all healthcare professionals, government agencies, non-governmental organisations, media and policymakers are also as important to achieve this necessary goal. Those who most affected by osteoporosis are our senior citizens who have contributed very much to the society and as a good and caring society it is our job to ensure our senior citizens is cared for the best we can.