Genital/Vulvovaginal Candidiasis is also sometimes called a “yeast infection.” It is a common infection that occurs when there is overgrowth of the yeast called Candida.
Most cases of Candida infection are caused by the person’s own Candida organisms. Candida yeasts usually live in the mouth, gastrointestinal tract, and vagina without causing symptoms. However, when an imbalance occurs, such as when the normal acidity of the vagina changes or when hormonal balance changes, Candida can multiply and build up. When this happens, symptoms of a “yeast infection” may appear. Less commonly, Candida infections can be passed from person to person through sexual intercourse.
Table of Contents
Oral yeast infection
Oral thrush is a condition in which the fungus Candida albicans accumulates on the lining of mouth. Candida is a normal organism in the mouth, but sometimes it can overgrow and cause symptoms.
Oral thrush causes creamy white lesions, usually on the tongue or inner cheeks. Although oral thrush can affect anyone, it’s more likely to occur in babies, the elderly, and in people with suppressed immune systems or certain health conditions, or those who take certain medications such as steroid.
What are the symptoms?
Symptoms of vulvovaginal candidiasis include:
- Itching, soreness and/or burning discomfort in the vagina and vulva
- Heavy white curd-like vaginal discharge
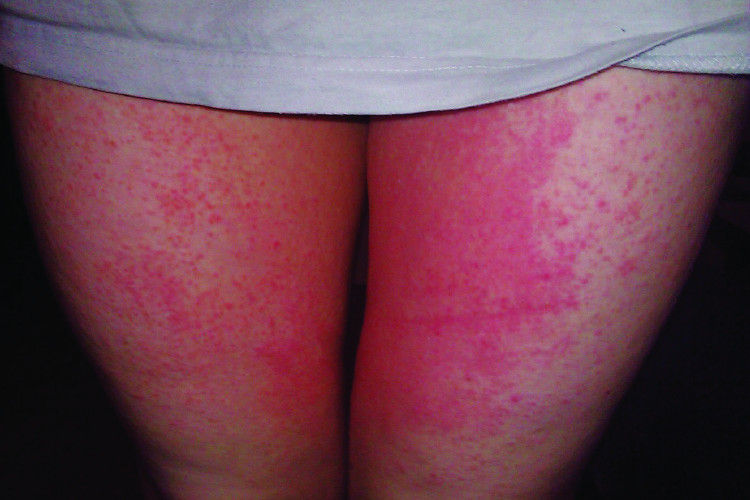
- Bright red rash affecting inner and outer parts of the vulva, sometimes spreading widely in the groin to include pubic areas, inguinal areas and thighs.
- Men with genital candidiasis may experience an itchy rash on the penis.
Who Gets Genital/Vulvovaginal Candidiasis?
Both men and women can get yeast infection, though it is more often associated with women.
Nearly 75% of all adult women have had at least one “yeast infection” in their lifetime.
On rare occasions, men can also get genital candidiasis. In men, it usually affects the head of the penis – causing irritation, discharge and redness.
Genital yeast infection occurs more frequently and more severely in people with weakened immune systems. Other conditions that may put a woman at risk for genital candidiasis include:
- Pregnancy
- Diabetes
- Long-term use of broad-spectrum antibiotics
- Use of corticosteroid medications
How can I prevent Genital/Vulvovaginal Candidiasis?
Wearing cotton underwear may help to reduce the risk of developing a yeast infection.
For women who experience recurrent yeast infections (more than three per year), some evidence suggests that oral or intravaginal probiotics may help to prevent frequent infections. However, consuming fermented foods doesn’t seem to reduce the risk of infection.
Should you see a doctor?
If you suspect yeast infection for the first time, it’s best to see a doctor for a diagnosis. This is because the symptoms can be similar to those of a sexually transmitted infection (STI). If you’ve had yeast infection before and you recognise the symptoms, you can treat it yourself with over-the-counter medication
Diagnosis
Usually the diagnosis is made on the basis of clinical features, the symptoms and the appearance of the skin lesion and vaginal secretion. The diagnosis may be further confirmed by taking a sample of the vaginal secretions and looking at the sample under a microscope to see if an abnormal number of Candida organisms are present.
How is Genital/Vulvovaginal Candidiasis treated?
General advice is to avoid local irritants e.g. perfumed products and tight fitting synthetic clothing. Several different antifungal medications are available to treat genital candidiasis. Antifungal vaginal suppositories or creams are commonly used. The duration of the treatment course of creams and suppositories can range from one day to seven days of therapy.
Mild or moderate infections can sometimes be treated with a single dose of oral antifungal medication, e.g. Fluconazole 150mg.
All topical and oral azole therapies give an 80-95% clinical and mycological cure rate in acute vulvo-vaginal candidiasis in non-pregnant women, but some people may have recurrent or resistant infections.
Recurrent vaginal yeast infection
Antibiotics are often implicated as a cause of recurrent vulvovaginal candidiasis. Frequent antibiotic use decreases protective vaginal flora and allows colonisation by Candida species.
Contraceptive methods may also promote recurrences of vulvovaginal candidiasis. Use of spermicidal jellies and creams increases susceptibility to infection by altering the vaginal flora and increasing the adhesion of Candida organisms. Women who take oral contraceptive pills have a higher rate of vulvovaginal candidiasis.
The role of sexual transmission is controversial. There is no evidence to support treatment of asymptomatic male sexual partners. No clinical trial has found that the treatment of male sexual partners prevents recurrences of vulvovaginal candidiasis in women.
Diabetes mellitus is often considered a predisposing factor for recurrent vulvovaginal candidiasis. Hyperglycemia enhances the ability of Candida albicans to bind to vaginal mucosal. However, unless other symptoms are suggestive of diabetes, patients with recurrent vulvovaginal candidiasis are rarely found to be diabetic.
Vaginal yeast infection in pregnancy
Vulvovaginal yeast infection is common during pregnancy and does not require treatment unless symptomatic. Intravaginal application of antifungal pessary such as clotrimazole, miconazole and econazole are commonly used. There have been no reported cases of foetal abnormalities with such treatment, which should be continued for at least seven days. Additional imidazole cream may be applied if vulvar symptoms are present. Oral antifungals should not be used. Diabetes should be considered if vaginal candidiasis is recurrent or complicated.