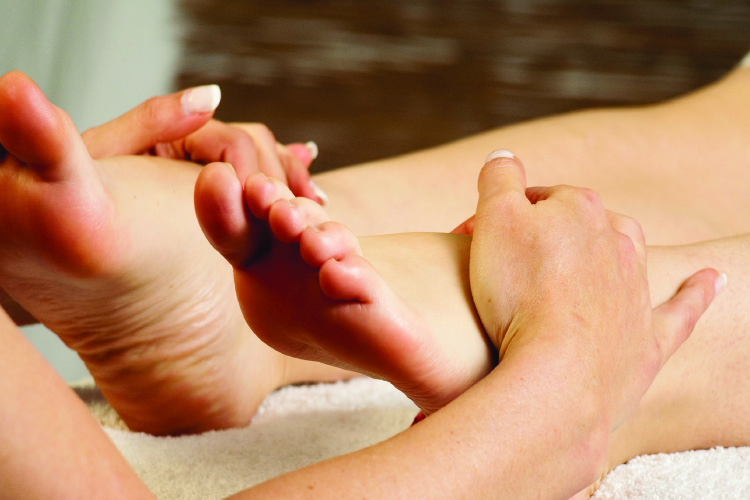
What causes cracked heels? And what are the best ways to avoid them?
Most of the foot problems arise due to neglect and oversight with regard to feet care. Cracked heels are the most common foot problem caused by dry skin complicated by callus formation (thickening and hardening of skin) around the rim of the heel. Cracked heels are not harmful in anyway, and for most people this is a nuisance and a cosmetic problem.
But when the cracks are deep, they are painful to stand on and the skin can bleed. In severe cases this can become infected. Wearing open or thin soled shoes usually worsen the symptoms. Some people are born with naturally dry skin that predisposes them to the cracks. The thickened dry skin (callus) around the heel that is more likely to crack is often due to mechanical factors that increase pressures in that area (e.g. wearing high heel or thin soled shoes).
Factors that can be involved in the cause of cracked heels include:
• prolonged standing (at work or home, especially on hard floors)
• continuous exposure to water (rob the skin of its natural oil)
• being overweight (this increases the pressure on the normal fat pad under the heel)
• open back on the shoes (this allows the fat under the heel to expand sideways and increases the pressure to crack)
• some medical conditions predispose to dry skin (e.g. diabetes, hypothyroid)
• dry skin conditions (e.g. psoriasis, eczema)
• ageing (skin lose elasticity with age)
Applying oil-based moisturising cream daily is useful to prevent crack heels. A pumice stone can be used to reduce the thickness callus. It is important to avoid open back shoes or thin soled shoes. Never try to reduce the callus yourself with a razor blade or a pair of scissors, as there is a risk of taking too much skin off and developing infection.
What causes varicose and spider veins – and the remedies for them?
Varicose veins and telangiectasia (spider veins) are the visible surface manifestations of an underlying problem with reverse venous flow, which is also termed venous insufficiency syndrome, caused by increased venous pressure. Normally, one-way valves in the vein keep our blood flowing towards the heart. In varicose and spider veins, the valves do not function properly; allowing blood to flow both ways, caused pooling of blood in the veins.
Varicose veins are dilated and tortuous veins due to an abnormal pooling of blood and affecting mostly women. Varicose veins are most common in the superficial veins of the legs, which are subject to high pressure when standing, although it may occur elsewhere. Besides cosmetic problems, varicose veins are often painful, especially when standing or walking. They often itch, and scratching them can cause ulcers.
Spider veins are small, twisted superficial veins most commonly affecting the face and legs. They can be red, purple or bluish in colour, and frequently sprawl out in a spider-web like pattern. Spider veins can appear in small patches where they are not very noticeable, or they can cover large areas of skin, resulting in an obviously unattractive appearance. They are similar to varicose veins, but very much smaller. In addition to being unsightly, spider veins can cause aching, heaviness, itching and night cramps.
Causes of varicose and spider veins include congenital defective valves from birth (hereditary), pregnancy and inflamed veins (thrombophlebitis). Standing for a long time and having increased pressure in the abdomen (e.g. obesity) may make you more likely to develop varicose veins. Trauma or injury to the skin, overexposure to ultraviolet rays and previous vein surgeries may also increase your risk of developing spider veins. Avoid prolonged standing and exercise regularly if personal or family history indicates you are at risk of developing varicose or spider veins.