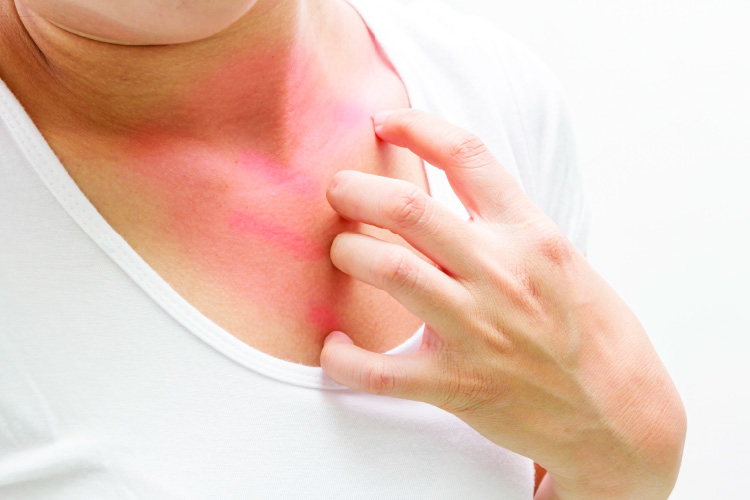
Eczema is a chronic inflammatory, relapsing and remitting skin disease that affects about 20% of children and 3% of adults. It is characterised by itching and scratching resulting in eczematous skin lesions. During the acute phase, the lesions are red, with blister formation and occasional oozing over a background of dry and scaly skin. However, persistent and chronic lesions tend to be associated with pigmentation and lichenification (thickened, hardened and rough skin texture).
The most common type of eczema is atopic eczema, a.k.a. atopic dermatitis (AD) which usually affects children, but can also affect adults. AD affects about one in 5 children and about one in 12 adults in the UK. In children, the onset often occurs between 3 and 6 months, with about 60% developing the condition before 1 year and 90% by 5 years of age. Most patients have personal or immediate family history of atopy (allergic rhinitis and asthma).
AD in infants usually present with rashes over the face and extensor areas with an underlying generalised dry skin. They usually improve remarkably between the ages of 2-5 years.
Childhood AD may follow infantile AD, or start between the age of 2 to 4 years. The rashes are often found in the creases of the neck, elbows, behind the knees and across the ankles. This form of AD usually improves with age. Although some children will outgrow their AD, most will continue to have dry and sensitive skin into adulthood.
It is estimated that approximately 10% of adolescents continue to suffer from eczema into adulthood.
Adult AD it is actually very similar to that of AD in older children. The areas of dry, itchy and reddened skin are predominantly at the neck, elbow creases, wrists, behind the knees and around the ankles.
Although the terms eczema and dermatitis are generally regarded as synonymous, not all eczema can be classified as atopic dermatitis. Eczema can be broadly categorised as exogenous or endogenous.
Table of Contents
Endogenous eczema
– conditions which are not a result of exogenous or external environmental factors, i.e. is mediated by processes originating within the body, most commonly atopic dermatitis (AD).
Exogenous eczemas
– conditions that are related to clearly defined external triggering factors, although inherited tendencies can also play a role. This group of disorder are broadly sub-categorised as:
Irritant contact dermatitis (ICD –occurs when chemicals or physical agents damage the surface of the skin faster than the skin is able to repair the damage. Irritants remove oils and moisture from the outer layer of the skin, allowing chemical irritants to penetrate more deeply and cause further damage by triggering inflammation.
Allergic contact dermatitis (ACD) – occurs when a material (allergen) comes in contact with the skin causing an allergic reaction. It arises some hours after contact with the allergen, and settles down over a few days, provided the allergen is removed from the skin.
Signs to watch out for
Pruritus is always intense, with significant effects on the activities of daily living, psychological disturbance and sleep. In adults, the disease affects different areas of the body compared to the infants. The hands, face and especially the eyelids are most often involved, in addition to skin creases and sometimes other areas. Inflammatory flare-ups can affect skin all over the body. This is called erythroderma.
These widespread conditions are serious, and can become more complicated when infections and metabolic disorders develop. They may require hospitalisation with a combination of intravenous, oral, topical therapies with intensive skin nursing care. Intravenous therapy includes intravenous steroids with antibiotic. Oral therapy is mainly anti histamine for itch control, whereas topical treatment encompasses emollients, steroid and antibiotic.
Why do some suffer while others don’t?
The exact cause of AD is complicated and not very clearly defined. It arises because of a complex interaction of genetic and environmental factors. Two important hypotheses have been proposed with regards to the development of inflammation leading to AD.
The first hypothesis suggests a primary immune dysfunction resulting in IgE sensitisation, while second hypothesis supports the theory of skin barrier disturbance.
The primary immune dysfunction results in an imbalance in the T-cell subsets, leading to massive production of inflammatory cytokines, causing an increase in circulating IgE.
The skin barrier dysfunction hypothesis suggests that AD patients develop AD as a result of skin barrier defects that allow for the entry of antigens, resulting in the production of inflammatory cytokines.
Furthermore, filaggrin mutations are associated with early-onset AD. One mechanism by which filaggrin defects may influence inflammation is by the release inflammatory cytokines.
How to alleviate the symptoms and remedies available:
- Avoidance of triggers known to aggravate the disease severity e.g. extremes of temperature
- clothes that contain wool or other irritant fibres
- harsh soaps and detergents
- keeping long finger nails
- contact with furry animals
- Keep your skin hydrated at all times as eczema is a disease characterised by impaired skin barrier function. Therefore, there is increased trans-epidermal water loss resulting in constant dry skin. Emollients are the cornerstone therapy for eczema management.
- As eczema is an inflammatory skin disease, topical steroids are important to reduce the inflammation and itch in addition to emollients.
- Topical immunomodulatory agents, e.g. tacrolimus and pimecrolimus, are suitable alternatives to topical corticosteroids especially at creases, face and genitalia as these agents do not cause skin atrophy.
- Anti-histamines are helpful for pruritus control and improve sleep at night.
Treat acute flares of eczema rapidly:
- Intermediate or high potency topical steroids for short periods of time to treat exacerbations.
- Oral or intravenous antibiotics as skin infections with Staphylococcus aureus may be a recurrent problem.
- Oral anti-viral therapy may be required if there is secondary viral skin infection e.g. herpes simplex virus.
When to seek medical help?
Patients diagnosed with eczema will be advised to be under the follow up with their dermatologists or general practitioner. This will improve long term care and monitor acute flares early during the course of disease.
Medical help is needed at different stages of disease:
Initial stage:
- Patients and their family members should be educated about the chronic nature of eczema, and most importantly the non-contagious nature of this condition.
- They should be aware of aggravating factors, and appropriate management to achieve effective control of their condition. This ensures cooperation and improved compliance which translates to better outcomes.
- Patients should be exposed to organisations and local support groups to receive up-to-date information about their condition.
Acute flares:
- Patients should be aware of the signs and symptoms of an impending flare of their condition.
- They may accelerate their therapy during the initial stage, but they must not hesitate to get professional support when they are unable to control the progression of disease.
- Different patients have different severity of disease and hence, therapy is catered for each individual patient