Early detection of breast cancer will save more lives. This is why your annual mammogram is important. However, the accuracy of your mammography is highly crucial as well. This is where 3D mammography comes in. A recent study published in JAMA (Journal of the American Medical Association) demonstrated that 3D mammography finds a 41 percent increase in the detection of invasive breast cancers and a 29 percent increase in the detection of all breast cancers as compared to conventional 2D mammography alone.
3D mammography can be performed for any women but is particularly beneficial for women with dense breasts, family history of breast cancer or other associated risk factors. In fact, this method is beginning to replace standard 2D mammography for cancer screening in many centres in the United States and Europe. Let’s take a look at how 3D mammography compares to the 2D version.
3D Mammography vs 2D Mammography
In 2D mammography, each breast is imaged twice through two compression methods, resulting in two static images for each breast – craniocaudal (CC) and mediolateral oblique (MLO). For 3D mammography (also known as digital breast tomosynthesis (DBT), multiple projections are obtained at predefined angles during the same compression methods, resulting in 3D-like or “volumetric” reconstruction of breast contents. Generally, 2D images can be acquired using a 3D machine but not vice versa.
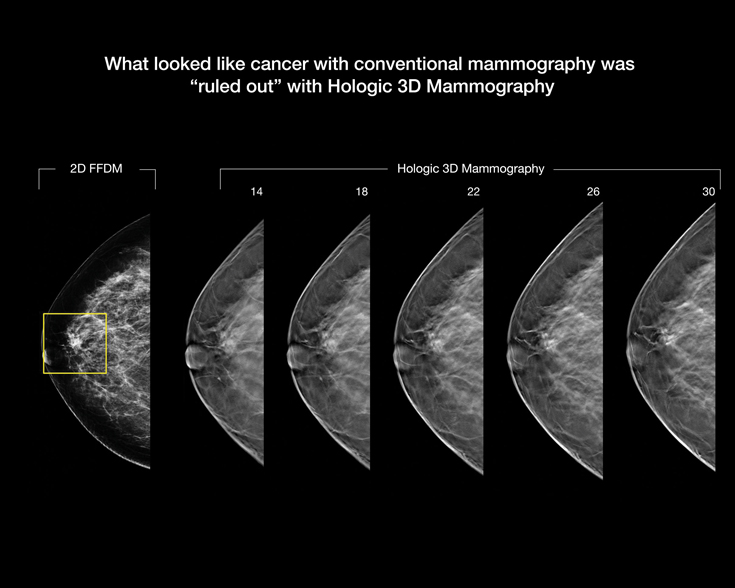
The greatest advantage of 3D mammography is its superior ability to distinguish occult lesions from the background of normal breast tissue. This is particularly useful for dense breast parenchyma patterns which may otherwise obscure tiny lesions in conventional 2D mammography. Numerous studies have also shown that 3D mammography results in significant increase in cancer detection rate, enhanced lesion detection, precise lesion localization and decreased recall rate compared to 2D mammography.
Radiation Levels
Both 2D and 3D exams utilise low-dose X-ray to visualise the structures inside the breasts. Effective radiation dose of 3D mammography is comparable to that of 2D mammography (approximately 0.5mSv versus 0.4mSv). To put it in perspective, the average worldwide annual background radiation dose stands at 2.4mSv/year.
As 3D mammography is fairly recent, many clinical trials are conducted using 3D exams in addition to standard 2D mammography, resulting in the often quoted 2 times radiation dose. However, with the promising development of synthetic tomosynthesis 2D images, conventional 2D mammography may no longer be required – potentially resulting in reduced radiation dose.
In 3D mammography, radiologists can view breast images in “slices,” which essentially allows them to see straight through tissue layers and makes it less likely they’ll miss an early sign of cancer.
Source: https://www.yalemedicine.org/conditions/3d-mammography/
A Simple Procedure
You will first be guided to the mammography suite by a female radiographer. During the procedure, as with 2D mammography, each of your breast will be compressed at two positions, resulting in a total of four compressions for both breasts.
Each compression will be followed by a moving X-ray tube making an arc over your breasts – each lasting no longer than 10 seconds. After the procedure is complete, your images will be sent to a computer to process the 2D and 3D images. The whole stack of images will be then be reviewed by a radiologist.

Consultant Clinical Radiologist
Sri Kota Specialist Medical Centre (SKSMC)
References:
- Ryusuke Murakami, et al. Comparative analysis between synthetic mammography reconstructed from digital breast tomosynthesis and full-field digital mammography for breast cancer detection and visibility. European Journal of Radiology Open. January 2020. 7:100207.
- Greeshma A. Agasthya, et al. Can breast compression be reduced in digital mammography and breast tomosynthesis? AJR Am J Roentgenol. 2017 Nov; 209(5):W322-W332.
- Per Skaane. Breast cancer screening with digital breast tomosynthesis. Breast Cancer. 2017 Jan;24(1):32-41.
- Sarah M Friedewald, et al. Breast cancer screening using tomosynthesis in combination with digital mammography. JAMA. 2014 Jun 25;311(24):2499-507.